More than three decades after the Genocide against the Tutsi in Rwanda, a significant portion of the population continues to grapple with its enduring effects on mental health.
Mukagaju (pseudonym), a survivor of the Genocide against the Tutsi, suffered from PTSD for 29 years. Although the genocide ended three decades ago, in her mind, it was still an ongoing nightmare. She continuously relived the harrowing scenes of screaming, running, hiding, and the killings she witnessed during the 100 days of horror. Due to the lack of appropriate support, she turned to prayer, hoping for healing, but to no avail.
"I was unable to sleep, suffered from terrible headaches, and was terrified of being alone. I would stay awake, hyper-alert throughout the night, hiding at the slightest sound or whenever I heard footsteps near my house, believing the perpetrators were coming for me and my children," she recounted.
Over the past three decades, the Government of Rwanda has made commendable strides in addressing the mental health burden by decentralising mental health and psychosocial support services to the health centre level and integrating them into primary healthcare.
However, national efforts face significant challenges, including insufficient funding, limited awareness and understanding of mental health, pervasive stigma, and a shortage of mental health professionals. The high prevalence of mental health conditions and the low utilisation of available services further exacerbate these issues.
The 2018 Rwanda Mental Health Survey (RMHS) by Rwanda Biomedical Centre (RBC) indicated a prevalence of mental disorders at 20.49%, substantially surpassing the global average. Today, that rate is likely higher than reported in 2018. In 2023, RBC reported that one in five Rwandans experiences mental health challenges, with 2,879 suicide attempts documented by the Health Management Information System (HMIS).
By June 2024, HMIS identified schizophrenia and other psychotic disorders (18%), depression (10%), bipolar disorder (2%), and Post-Traumatic Stress Disorder (PTSD) (2%) as the most common diagnoses. Globally, it is projected that by 2030, mental health disorders—particularly depression—will rank as the leading contributor to the global burden of disease. Furthermore, the intergenerational trauma stemming from the genocide continues to jeopardise the mental well-being of younger generations. Despite the high prevalence of mental health conditions, only 5.6% of the population seeks services from formal mental health care systems, according to RMHS.

According to Rwanda’s health workforce statistics, the country has only 16 psychiatrists (a ratio of 1 per 862,400 people), 441 certified clinical psychologists (1 per 31,289 people), and 202 mental health nurses (1 per 68,400 people) working in public facilities. These professionals primarily employ a one-on-one approach and often prioritise pharmacological treatments over psychotherapy.
Mukagaju eventually overcame her trauma after joining a Resilience-Oriented Therapy healing group established at Rukira Health Centre in Ngoma District, Eastern Province of Rwanda, six months ago. “Today, I sleep peacefully after years of fear and hypervigilance. Nothing frightens me to the point of fleeing my home at night, because now I know we are not in the middle of the genocide. I’ve learned to control my fears whenever they arise,” she joyfully explained.
Resilience-Oriented Therapy is a psychological intervention designed to address mental health issues related to emotional regulation, identity development, behavioural self-management, and the enhancement of individual psychological resilience within a group setting. Introduced in health centres in October 2023 through a joint effort by Interpeace and the Government of Rwanda, spearheaded by RBC, the therapy aims to provide a sustainable, cost-effective solution to the challenges posed by the high prevalence of mental health disorders.
Resilience-Oriented Therapy not only addresses mental health issues rooted in traumatic events such as the genocide but also supports individuals facing conditions triggered by various life circumstances. For instance, Uwimana (Pseudonym), who attempted suicide twice due to depression after suffering mistreatment from her husband—who abandoned her while she was four months pregnant—shared her transformative experience.
"I tried to throw myself and my children into the river because I thought ending our lives was the only way out of my pain. I didn’t want to have another child after being abandoned. This group has helped me; I no longer feel stressed or depressed. I’ve found inner peace, and now I am determined to raise my children with hope for a brighter future," Uwimana said, holding her five-month-old baby, who she noted would not have been born had she not joined the Resilience-Oriented Therapy group at Nyakigezi Health Centre, Rugera Sector, Nyabihu District, Western Province.
Resilience-Oriented Therapy represents the first group-based intervention introduced within formal health facilities in Rwanda. It is currently available in 32 health centers and seven district hospitals across five districts—Musanze, Ngoma, Nyabihu, Nyagatare, and Nyamagabe—and is administered by trained psychologists or mental health nurses. To date, 446 individuals (308 women and 138 men) have benefited from the therapy.
The therapy is tailored to Rwanda’s specific cultural context, while incorporating international best practices, ensuring its relevance and effectiveness.
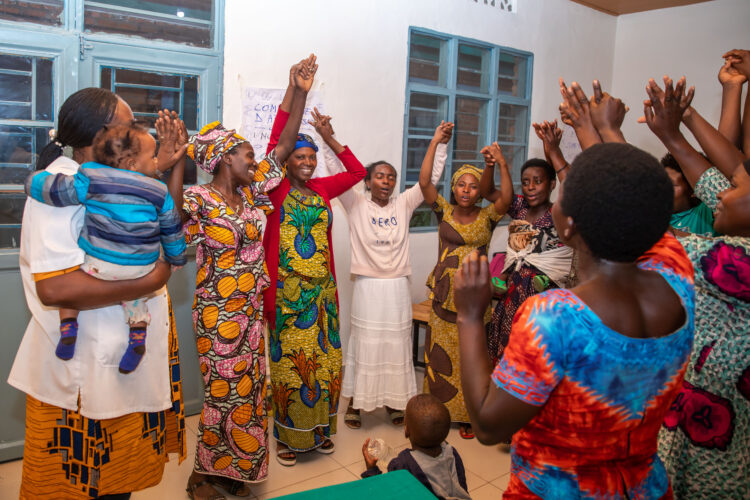
The healing process spans six months, with the group convening for weekly three-hour sessions. Through this intervention, participants acquire psychosocial skills for trauma management, emotional regulation, self-care, and resilience building, equipping them to navigate daily challenges and adapt to evolving circumstances.
Dr. Jean Damascene Iyamuremye, Director of Psychiatric Care at RBC, recognises the positive impact Resilience-oriented therapy has had on the community and advocates for its nationwide expansion. "This is an innovative approach compared to the one-on-one approach we have been using. We have observed considerable progress since its implementation. In the community, people are now more motivated to seek professional help at the early stages of their mental health challenges. They have found healing and solace, and our hope is to scale this therapy across the country. It’s a community-based intervention we deeply appreciate, as it has also enhanced the overall quality of care,” Dr. Iyamuremye remarked. Interpeace is working with RBC to scale up the intervention across the country.
A recent study testing Multifamily Healing Spaces (MFHS), a new psychological intervention approach for families, has shown strong effectiveness in resolving intrafamily conflicts, enhancing communication and problem-solving skills, and building family cohesion and resilience. The intervention also addresses the intergenerational trauma through parent-child dialogues and promotes positive parenting.
The study, a Randomised Controlled Trial (RCT) conducted between April and September 2023, assessed MFHS, a group-based psychosocial tool designed to help families confront historical traumas, improve communication, and resolve conflicts through healing dialogues. MFHS blends home-grown solutions with international best practices, tailored to the Rwandan context.
The MFHS approach was introduced as part of the societal healing programme titled “Reinforcing Community Capacity for Social Cohesion and Reconciliation through Societal Trauma Healing in Rwanda,” jointly implemented by Interpeace and local partners—Prison Fellowship Rwanda, Dignity in Detention, and Haguruka—in collaboration with the Ministry of National Unity and Civic Engagement (MINUBUMWE) and the Ministry of Health via the Rwanda Biomedical Centre (RBC). The programme is funded by the Government of Sweden.
The Genocide against the Tutsi, three decades ago, not only devastated individuals but also shattered family structures and the fabric of family life in Rwanda. Families continue to grapple with the trauma of the genocide and its aftermath, compounded by the intergenerational transmission of genocide-related legacies, which has become a significant societal challenge. This is further exacerbated by social pressures as Rwanda strives for socioeconomic development, aiming to become a middle-income country by 2035 and a high-income country by 2050.

For Rwanda to achieve sustainable peace and development, it must prioritise healthy families, as they are the foundation of society. Yet, many families still face challenges that undermine cohesion and development. According to the Rwanda Governance Board (RGB) Citizen Scorecard report 2023, family conflict is the top challenge to family cohesion (22.3%), followed by extramarital affairs (17.2%), psychological violence (16.1%), and economic violence (14.4%). Additional issues include physical violence (8.8%) and juvenile delinquency (8.4%).
The 2023 RGB Citizen Scorecard report identifies alcohol abuse as the leading cause of family dysfunction (85.4%), followed by poor communication between family members (81.3%) and poor parenting (58.9%). These problems negatively impact family members' mental well-being, pushing some toward substance abuse, which further hinders their participation in economic activities, ultimately leading to poor livelihoods.
The Randomised Controlled Trial (RCT) was conducted with the aim to develop and evaluate a family-based intervention promoting a multisystemic approach to resilience at personal, family, and community levels, with three key objectives: strengthening family resilience, facilitating personal transformation, and restoring community trust.
A total of 95 families (283 individuals: 136 males, 147 females) from Nyagatare, Ngoma, Nyamagabe, Nyabihu, and Musanze participated. These families included genocide survivors, genocide perpetrators, ex-combatants, and returnees, all coming from disharmonious families. They were divided into 20 groups: 9 treatment groups (146 participants) and 11 control groups (137 participants). Parents and children in treatment groups participated in 18 weeks of healing dialogues in a group setting, followed by six weeks of follow-up, while the control group was placed on a waiting list. Groups were established in their communities and facilitated by two well-trained Community Dialogue Facilitators, selected from their community and whom they trust. Post-intervention data from both groups were compared with baseline data to measure the treatment's impact.
The findings revealed that MFHS significantly enhanced family resilience, with improvements in family belief systems, communication, problem-solving skills, and organizational patterns. Families in the treatment groups demonstrated a more constructive approach to deal with challenges, showcasing stronger teamwork and mutual support compared to the control group.
Regarding partner dynamics, the intervention positively affected collaboration and relationship among couples in the treatment group, reflecting improved happiness and satisfaction within the family. Couples as both partners and parents acquired social and emotional management skills which enabled them to address existing conflicts, and strengthen bonds, and develop strategies for handling future conflicts and challenges.

“I felt traumatized by the violence of my husband, as he used to beat me almost every day. I had no rights to the family property and was treated like a maid. In this group, we learned to discuss and resolve our problems as a family. He even acknowledged his misdeeds and apologised to me. I can’t imagine what would have happened if we hadn’t joined the multifamily healing dialogues,” said a participant from Nyabihu District. She added that her husband has since changed, becoming a caring husband and father who now consults her before making decisions.
The intervention also promoted positive parenting, with those in the treatment group reporting higher levels of authoritative-democratic and authoritative-warm parenting styles, which prioritise guidance and involvement of children compared to the control group, who continued to adopt authoritarian style where parents are extremely rigid and use tough rules and punishments to control their children. Through parent-child sessions, families engaged in open discussions about daily life, historical trauma, and the history of the Genocide against the Tutsi, leading to a shared vision for the future.
The findings also reveal that the intervention had additional positive impacts beyond the expected results. Families in the treatment groups significantly improved their livelihoods by learning to better manage family resources and work together toward shared goals.
A study conducted to test a new psychological intervention – Resilience-oriented therapy (ROT)- has revealed its strong effectiveness in addressing mental health issues related to emotional regulation, identity development, and behavioural self-management as well as strengthening individual psychological resilience in Rwanda.
The Randomised Controlled Trial (RCT) - a prospective study that serves to measure the effectiveness of a new intervention or treatment - was conducted between April and September 2023 to test the effectiveness of ROT, a group-based, strengths-based and trauma-informed modular treatment protocol designed in the framework of the societal healing programme titled “Reinforcing Community Capacity for Social Cohesion and Reconciliation through Societal Trauma Healing Rwanda” jointly implemented by Interpeace and its local partners – Prison Fellowship Rwanda, Dignity in Detention and Haguruka – in close collaboration with the Ministry of Health through Rwanda Biomedical Centre (RBC) and the Ministry of National Unity and Civic Engagement (MINUBUMWE). The programme is funded by the Government of Sweden through its Embassy in Rwanda.
A significant proportion of Rwandans is still grappling with mental health issues stemming from the Genocide against the Tutsi. The Rwanda Mental-Health Survey (2018) revealed that the prevalence of several mental difficulties in the general population stands at 20.49% and is significantly higher than the global average with major depression being the most prevalent mental disorder (12.0%). Genocide survivors are the most affected (52%). Rwanda has made commendable strides in curbing and treating mental health issues and decentralising mental health and psychosocial support service care at the health centre level as well as integrating it into primary care.

Nevertheless, the scale of needs still outstrips the capacity of available professionals and infrastructure.
The country has only 16 psychiatrics (1 for 862,400 persons), 441 certified clinical psychologists (1 for 31,289 persons) and 202 mental health nurses (1 for 68,400 persons) working in public facilities. implementing a one-on-one approach and often prioritising medication over psychotherapy treatment. Additionally, there are just seven private clinics or hospitals offering mental health services.
In a collectivistic society like Rwanda, the one-on-one interventional approach – largely implemented across the country - does not enable professionals to provide cost-effective service. The utilisation of mental-health services remains low standing at only 5.3%.
ROT intervention protocol was developed to adequately respond to the existing gaps and support the Rwandan Government’s efforts in promoting mental health care provision for all. Its design blended the emerging international best practices with Rwandan context-specific tools to adapt it to the actual realities of the country.
The RCT study of ROT involved 394 community members (146 male and 248 female) selected from five districts, namely Nyagatare, Ngoma, Nyamagabe, Nyabihu and Musanze. After collecting pre-intervention data through a baseline assessment, participants were allocated into 49 groups falling under two categories: treatment (25 groups) with 211 participants and control (24 groups) with 181 participants.
Those who were allocated to treatment groups received ROT intervention in a group setting through 24 therapy sessions for a period of three months, followed by six weeks of follow up sessions. Group members met two times a week and engaged in healing dialogues facilitated by certified psychologists or mental health nurses who were assisted by trained counsellors. Those who were allocated into control group were put on a waiting list.
Post-intervention data were collected from both treatment and control groups and compared with baseline data and crosschecked to ascertain the effectiveness of the approach. The findings showed a significant increase in psychological resilience of participants who received the treatment while those in the control groups (waiting list) reported a decrease in resilience. The comparison between pre- and post-invention data demonstrated that depression rates dropped from 8.1 (22.5%) to 2.9 (8%), anxiety from 13.4 (33.5%) to 6.3 (15.7%), and borderline personality disorders from 4.5 (11.3%) to 2.6 (6.5%) among treatment group members.

The findings further indicated that the intervention significantly improved self-management skills, emotional well-being skills, collaboration skills and personal agency. Individuals in the treatment demonstrated enhanced capacity for adapting to changes, and effectively navigating life's challenges.
“My life was shrouded in darkness, and I couldn't see any hope for the future. I felt lost and isolated in my own world. Each day was a struggle, and despair seemed to be my constant companion. The Resilience-oriented therapy group became the turning point in my life. It provided me with a conducive environment and safe space where I could heal and grow. I learned how to face life's challenges head-on, how to bounce back from setbacks, and most importantly, how to cultivate a resilient mindset,” said a female Genocide survivor from Rukumberi Sector, Ngoma District who received ROT.
The intervention appears to have also had a small but promising effect on alcohol abuse and drug dependency. Those who were in treatment groups reported to have, at least significantly reduced alcohol intake. Findings also showed a promising effect in reducing aggression.
Mental health professionals commend ROT as an empirically validated cost-effective intervention for addressing various mental health difficulties and strengthening the resilience of individuals. “Resilience-oriented therapy connects people, enabling them to support each other in their journey of healing and resilience,” said Prof. Eugene Rutembesa, a university lecturer in clinical psychology at the University of Rwanda. He has incorporated this therapy into his lectures and advocates for its integration into the university curriculum to facilitate its wide dissemination and use.
Interpeace will participate at COP29 in Baku, Azerbaijan to spark innovative thinking around peace-positive climate adaptation and mitigation approaches to unlock greater climate action and finance in conflict-affected and fragile contexts.
Developing countries and conflict-affected areas bear the brunt of climate risks. Yet, only 20 to 25% of the $1.5 trillion in climate investments needed are funded, and development finance is providing less than 6% of the rate required.
The Peace, Relief, and Recovery Day on 15 November is a key opportunity to ignite policy and advocacy around the climate-peace nexus, including initiatives such as the Call on Climate Action for Peace, Relief and Recovery endorsed by Interpeace, and the Baku Climate and Peace Action Hub announced by the COP29 Presidency.
Highlights of the delegation’s activities in Baku include a panel organised jointly with the IOM on November 13, focusing on the need to strengthen partnerships between development finance institutions, the UN, and peacebuilding actors, to extend the reach of climate finance in countries most impacted by climate shocks and conflict. With the ISO, we will also advocate for the importance of positioning international standards as essential tools to ensure policy alignment, facilitate global cooperation, and enable collective action on critical issues.
Interpeace will engage bilaterally with member-states, multilateral climate funds and development finance actors, the private sector and impact investors, and civil society representatives to explore concrete ways to operationalize the pledges, regional and cross-regional initiatives recognising the interlinks between climate and peace, such as the landmark Declaration on Climate, Relief, Recovery and Peace launched at COP28 in the presence of Interpeace President Itonde Kakoma.

Learn more about the event Cliquez ici.
It was a full house on Thursday 3 October at the event in Nairobi as Interpeace launched its research “Entry-Points for Peace-Positive Investments in Northern Kenya’s Frontier Markets – An exploratory study of prospective peace-aligned investments in Elgeyo Marakwet, Mandera and Marsabit counties”. The event brought together the national and regional government, investors, peacebuilders, development actors and CSOs to outline next steps in order to attract peace-positive investment to Northern Kenya.
Member of Interpeace’s Governing Board Ambassador Amina Mohamed said: “Today marks a pivotal moment in our shared journey towards fostering stability and sustainable development in Northern Kenya. Through collective efforts we can unlock transformative change.”
Ambassador Mohammed outlined the importance of initiatives such as Finance for Peace by Interpeace, as the organisation has played a pivotal role in strengthening the capacity of local communities to manage conflicts and promote social cohesion. “These efforts”, she said, “have reshaped community relationships, reduced violence and nurtured trust among diverse stakeholders.
“As we navigate towards inclusive investment strategies, the concept of Peace Finance becomes paramount. By integrating peace efforts into our investment frameworks we can mitigate risks, enhance returns and contribute significantly to a peaceful and prosperous Northern Kenya”, Ambassador Mohammed said.
Full speech: https://shorturl.at/Trjo1

Principal Secretary of the State Department for Devolution Ms Terry Mbaika affirmed the Kenyan Government’s commitment to promote peace-positive investments in the country. She said: “It is clear that peacebuilding considerations need to be better integrated into development finance and mainstreamed into investment approaches.
“The Government is committed to integrating peace initiatives into its development agenda. We do this by ensuring that every step towards economic growth is accompanied by conscious efforts to maintain and enhance stability.” Ms Mbaika called for the alignment of investment opportunities with peacebuilding efforts to create mutual benefits for both investors and local communities.
Full speech: https://shorturl.at/YxdSZ

Michael Pietsch of the German Embassy in Kenya said: "Germany is spearheading financing for peace. We need to ensure investments positively impact peace. We need Finance for Peace. Germany is partnering with Interpeace to develop a Peace Finance Impact Framework and Peace Finance Standard.
“Protracted conflicts across the globe have impeded development efforts and have led the UN Secretary-General to call upon the international community to intensify efforts for peace and identify new sources for financing for peace. Recently, UN Member States reiterated their commitment to building and sustaining peace when endorsing the Pact for the Future. However, public resources are scarce and we need more sustainable financing for peace.”
Full speech: https://shorturl.at/vrlun

